Video: Watch a hair restoration specialist explain the DHT-follicle connection and what it means for treatment options.
It’s Not Just Genes: The Other Major Causes
While AGA is the leading cause, it doesn’t tell the whole story. Hair loss in men can also result from a range of other factors — some temporary, some serious. Here’s what the research says:

Telogen Effluvium: When Stress Pulls the Trigger
Telogen effluvium (TE) is considered the second most common form of hair loss seen by dermatologists (Healthline, 2023). It occurs when a significant physical or emotional stressor — think surgery, illness, extreme psychological pressure, or even COVID-19 — shocks a large number of hair follicles into the resting (telogen) phase of the hair growth cycle simultaneously (Phillips et al., 2017; Mayo Clinic, 2026).
The result? Handfuls of hair falling out, typically two to three months after the triggering event. The good news is that telogen effluvium is usually temporary. Once the stressor is resolved, hair typically regrows within six to nine months (AAD, 2023; Healthline, 2023). The bad news: chronic stress can turn what was once a temporary issue into a long-term problem.
Nutritional Deficiencies: You Are What You Eat — Including Your Hair
Your hair follicles are among the most metabolically active structures in the body. They require a constant, adequate supply of nutrients to maintain healthy growth cycles. Deficiencies in iron, zinc, protein, biotin, vitamin B12, and vitamin D have all been linked to hair loss and disrupted hair growth (AAD, 2023; Healthline, 2024).
According to Guo and Katta (2017), nutrient deficiency plays a meaningful role in hair loss, with iron deficiency being particularly prevalent among those experiencing diffuse shedding. The key takeaway: a nutritional gap doesn’t cause male pattern baldness, but it can dramatically accelerate it or trigger a separate shedding event altogether. If you’re looking to address this proactively, understanding the essential nutrients your follicles actually need is a good place to start.
Thyroid Disorders and Medical Conditions
Your thyroid gland produces hormones that regulate metabolism — and when those hormone levels are off, your hair pays the price. Both hypothyroidism (underactive thyroid) and hyperthyroidism (overactive thyroid) can cause diffuse hair thinning and loss (Mayo Clinic, 2026; Healthline, 2024).
Other medical conditions associated with hair loss include lupus, scalp psoriasis, polycystic ovary syndrome (PCOS) in women, and sexually transmitted infections like untreated syphilis (AAD, 2023).
Alopecia Areata: When the Immune System Turns Against You
Alopecia areata is a distinct autoimmune condition in which the body’s immune system mistakenly attacks healthy hair follicles, resulting in sudden, patchy hair loss (Mayo Clinic, 2026; AAD, 2023). It can affect the scalp, eyebrows, eyelashes, and other body hair, and in severe cases can lead to complete hair loss on the scalp (alopecia totalis) or across the entire body (alopecia universalis). Unlike androgenetic alopecia, alopecia areata is not driven by DHT but by immune dysregulation.
Medications and Chemical Treatments
A number of commonly prescribed medications list hair loss as a side effect. These include anticoagulants, anticonvulsants, beta-blockers, oral retinoids, and certain antidepressants (Healthline, 2024; Phillips et al., 2017). Hair loss related to medication typically resolves once the drug is discontinued, but always consult your doctor before stopping any prescription medication. For a fuller breakdown of which drugs are most commonly implicated, see our guide on prescription drug hair loss in men.
On the styling side, harsh chemical treatments — relaxers, perms, bleaching agents — can damage the hair shaft and, over time, scar hair follicles, leading to permanent loss (AAD, 2023).
Traction Alopecia: Your Hairstyle Could Be the Problem
If you regularly wear your hair in tight braids, man buns, or cornrows, the sustained tension on the hair shaft can cause traction alopecia — a form of hair loss caused by physical pulling of the follicle (Mayo Clinic, 2026; AAD, 2023). Unlike most other forms of hair loss, traction alopecia is entirely preventable by loosening hairstyles before permanent follicular scarring occurs.
Is Hair Loss Preventable?
The honest answer depends on the cause. Most hereditary hair loss — driven by DHT and genetics — is not preventable (Mayo Clinic, 2026). However, treatment started early can significantly slow the process. FDA-approved options like minoxidil (Rogaine) and finasteride (Propecia) have demonstrated efficacy in slowing hair loss and in some cases stimulating regrowth (Healthline, 2024; Phillips et al., 2017). For a detailed look at how these treatments compare and what the evidence actually shows, see our hair loss medications guide.
For non-hereditary causes, prevention is often very much possible: eating a nutrient-dense diet, managing stress, treating underlying medical conditions, and choosing gentler hairstyles can all meaningfully reduce hair loss risk (AAD, 2023; Mayo Clinic, 2026).
When Should You See a Doctor?
See a healthcare provider — ideally a dermatologist — if you notice sudden or patchy hair loss, shedding accompanied by scalp pain or itching, or hair loss following a new medication or significant health event (Mayo Clinic, 2026). Early intervention generally yields the best results, regardless of cause.
The Bottom Line
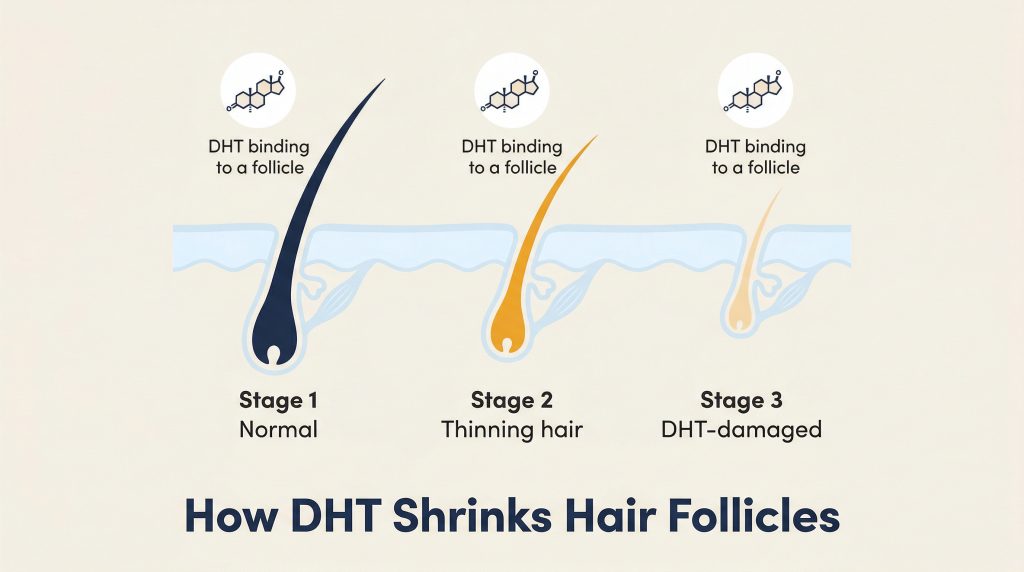
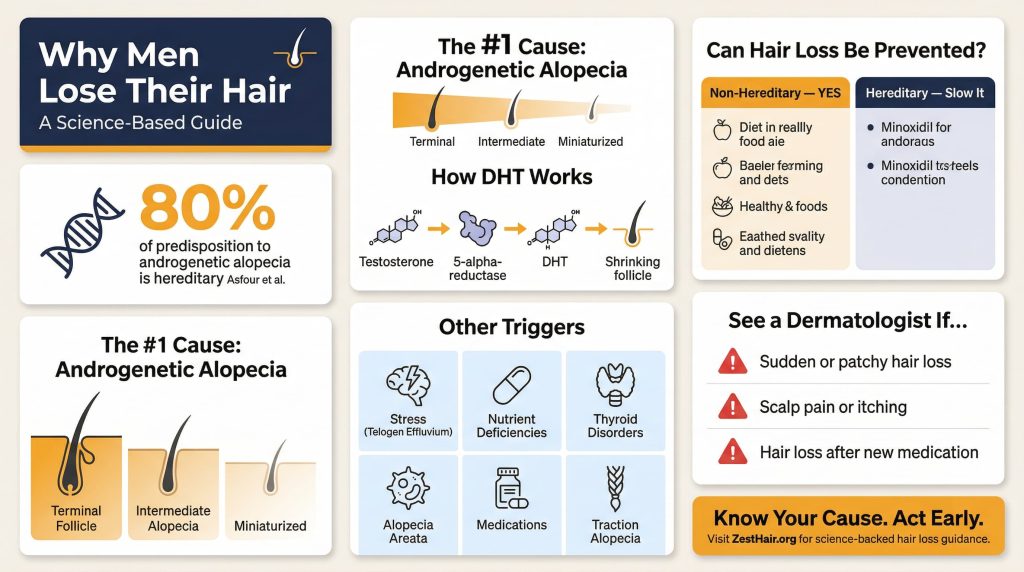
The main cause of hair loss in men is androgenetic alopecia — a hereditary condition driven by genetic sensitivity to DHT that causes progressive follicular miniaturization over time. It affects tens of millions of men and is responsible for the vast majority of male pattern baldness cases worldwide. But hair loss is rarely a single-factor story. Stress, nutritional gaps, medical conditions, autoimmune responses, and even the way you wear your hair can all compound or trigger hair loss independently.
Understanding the root cause — quite literally — is the first and most important step toward doing something about it.

Video: Watch a hair restoration specialist explain the DHT-follicle connection and what it means for treatment options.
It’s Not Just Genes: The Other Major Causes
While AGA is the leading cause, it doesn’t tell the whole story. Hair loss in men can also result from a range of other factors — some temporary, some serious. Here’s what the research says:

Telogen Effluvium: When Stress Pulls the Trigger
Telogen effluvium (TE) is considered the second most common form of hair loss seen by dermatologists (Healthline, 2023). It occurs when a significant physical or emotional stressor — think surgery, illness, extreme psychological pressure, or even COVID-19 — shocks a large number of hair follicles into the resting (telogen) phase of the hair growth cycle simultaneously (Phillips et al., 2017; Mayo Clinic, 2026).
The result? Handfuls of hair falling out, typically two to three months after the triggering event. The good news is that telogen effluvium is usually temporary. Once the stressor is resolved, hair typically regrows within six to nine months (AAD, 2023; Healthline, 2023). The bad news: chronic stress can turn what was once a temporary issue into a long-term problem.
Nutritional Deficiencies: You Are What You Eat — Including Your Hair
Your hair follicles are among the most metabolically active structures in the body. They require a constant, adequate supply of nutrients to maintain healthy growth cycles. Deficiencies in iron, zinc, protein, biotin, vitamin B12, and vitamin D have all been linked to hair loss and disrupted hair growth (AAD, 2023; Healthline, 2024).
According to Guo and Katta (2017), nutrient deficiency plays a meaningful role in hair loss, with iron deficiency being particularly prevalent among those experiencing diffuse shedding. The key takeaway: a nutritional gap doesn’t cause male pattern baldness, but it can dramatically accelerate it or trigger a separate shedding event altogether. If you’re looking to address this proactively, understanding the essential nutrients your follicles actually need is a good place to start.
Thyroid Disorders and Medical Conditions
Your thyroid gland produces hormones that regulate metabolism — and when those hormone levels are off, your hair pays the price. Both hypothyroidism (underactive thyroid) and hyperthyroidism (overactive thyroid) can cause diffuse hair thinning and loss (Mayo Clinic, 2026; Healthline, 2024).
Other medical conditions associated with hair loss include lupus, scalp psoriasis, polycystic ovary syndrome (PCOS) in women, and sexually transmitted infections like untreated syphilis (AAD, 2023).
Alopecia Areata: When the Immune System Turns Against You
Alopecia areata is a distinct autoimmune condition in which the body’s immune system mistakenly attacks healthy hair follicles, resulting in sudden, patchy hair loss (Mayo Clinic, 2026; AAD, 2023). It can affect the scalp, eyebrows, eyelashes, and other body hair, and in severe cases can lead to complete hair loss on the scalp (alopecia totalis) or across the entire body (alopecia universalis). Unlike androgenetic alopecia, alopecia areata is not driven by DHT but by immune dysregulation.
Medications and Chemical Treatments
A number of commonly prescribed medications list hair loss as a side effect. These include anticoagulants, anticonvulsants, beta-blockers, oral retinoids, and certain antidepressants (Healthline, 2024; Phillips et al., 2017). Hair loss related to medication typically resolves once the drug is discontinued, but always consult your doctor before stopping any prescription medication. For a fuller breakdown of which drugs are most commonly implicated, see our guide on prescription drug hair loss in men.
On the styling side, harsh chemical treatments — relaxers, perms, bleaching agents — can damage the hair shaft and, over time, scar hair follicles, leading to permanent loss (AAD, 2023).
Traction Alopecia: Your Hairstyle Could Be the Problem
If you regularly wear your hair in tight braids, man buns, or cornrows, the sustained tension on the hair shaft can cause traction alopecia — a form of hair loss caused by physical pulling of the follicle (Mayo Clinic, 2026; AAD, 2023). Unlike most other forms of hair loss, traction alopecia is entirely preventable by loosening hairstyles before permanent follicular scarring occurs.
Is Hair Loss Preventable?
The honest answer depends on the cause. Most hereditary hair loss — driven by DHT and genetics — is not preventable (Mayo Clinic, 2026). However, treatment started early can significantly slow the process. FDA-approved options like minoxidil (Rogaine) and finasteride (Propecia) have demonstrated efficacy in slowing hair loss and in some cases stimulating regrowth (Healthline, 2024; Phillips et al., 2017). For a detailed look at how these treatments compare and what the evidence actually shows, see our hair loss medications guide.
For non-hereditary causes, prevention is often very much possible: eating a nutrient-dense diet, managing stress, treating underlying medical conditions, and choosing gentler hairstyles can all meaningfully reduce hair loss risk (AAD, 2023; Mayo Clinic, 2026).
When Should You See a Doctor?
See a healthcare provider — ideally a dermatologist — if you notice sudden or patchy hair loss, shedding accompanied by scalp pain or itching, or hair loss following a new medication or significant health event (Mayo Clinic, 2026). Early intervention generally yields the best results, regardless of cause.
The Bottom Line
The main cause of hair loss in men is androgenetic alopecia — a hereditary condition driven by genetic sensitivity to DHT that causes progressive follicular miniaturization over time. It affects tens of millions of men and is responsible for the vast majority of male pattern baldness cases worldwide. But hair loss is rarely a single-factor story. Stress, nutritional gaps, medical conditions, autoimmune responses, and even the way you wear your hair can all compound or trigger hair loss independently.
Understanding the root cause — quite literally — is the first and most important step toward doing something about it.


Video: Watch a hair restoration specialist explain the DHT-follicle connection and what it means for treatment options.
It’s Not Just Genes: The Other Major Causes
While AGA is the leading cause, it doesn’t tell the whole story. Hair loss in men can also result from a range of other factors — some temporary, some serious. Here’s what the research says:

Telogen Effluvium: When Stress Pulls the Trigger
Telogen effluvium (TE) is considered the second most common form of hair loss seen by dermatologists (Healthline, 2023). It occurs when a significant physical or emotional stressor — think surgery, illness, extreme psychological pressure, or even COVID-19 — shocks a large number of hair follicles into the resting (telogen) phase of the hair growth cycle simultaneously (Phillips et al., 2017; Mayo Clinic, 2026).
The result? Handfuls of hair falling out, typically two to three months after the triggering event. The good news is that telogen effluvium is usually temporary. Once the stressor is resolved, hair typically regrows within six to nine months (AAD, 2023; Healthline, 2023). The bad news: chronic stress can turn what was once a temporary issue into a long-term problem.
Nutritional Deficiencies: You Are What You Eat — Including Your Hair
Your hair follicles are among the most metabolically active structures in the body. They require a constant, adequate supply of nutrients to maintain healthy growth cycles. Deficiencies in iron, zinc, protein, biotin, vitamin B12, and vitamin D have all been linked to hair loss and disrupted hair growth (AAD, 2023; Healthline, 2024).
According to Guo and Katta (2017), nutrient deficiency plays a meaningful role in hair loss, with iron deficiency being particularly prevalent among those experiencing diffuse shedding. The key takeaway: a nutritional gap doesn’t cause male pattern baldness, but it can dramatically accelerate it or trigger a separate shedding event altogether. If you’re looking to address this proactively, understanding the essential nutrients your follicles actually need is a good place to start.
Thyroid Disorders and Medical Conditions
Your thyroid gland produces hormones that regulate metabolism — and when those hormone levels are off, your hair pays the price. Both hypothyroidism (underactive thyroid) and hyperthyroidism (overactive thyroid) can cause diffuse hair thinning and loss (Mayo Clinic, 2026; Healthline, 2024).
Other medical conditions associated with hair loss include lupus, scalp psoriasis, polycystic ovary syndrome (PCOS) in women, and sexually transmitted infections like untreated syphilis (AAD, 2023).
Alopecia Areata: When the Immune System Turns Against You
Alopecia areata is a distinct autoimmune condition in which the body’s immune system mistakenly attacks healthy hair follicles, resulting in sudden, patchy hair loss (Mayo Clinic, 2026; AAD, 2023). It can affect the scalp, eyebrows, eyelashes, and other body hair, and in severe cases can lead to complete hair loss on the scalp (alopecia totalis) or across the entire body (alopecia universalis). Unlike androgenetic alopecia, alopecia areata is not driven by DHT but by immune dysregulation.
Medications and Chemical Treatments
A number of commonly prescribed medications list hair loss as a side effect. These include anticoagulants, anticonvulsants, beta-blockers, oral retinoids, and certain antidepressants (Healthline, 2024; Phillips et al., 2017). Hair loss related to medication typically resolves once the drug is discontinued, but always consult your doctor before stopping any prescription medication. For a fuller breakdown of which drugs are most commonly implicated, see our guide on prescription drug hair loss in men.
On the styling side, harsh chemical treatments — relaxers, perms, bleaching agents — can damage the hair shaft and, over time, scar hair follicles, leading to permanent loss (AAD, 2023).
Traction Alopecia: Your Hairstyle Could Be the Problem
If you regularly wear your hair in tight braids, man buns, or cornrows, the sustained tension on the hair shaft can cause traction alopecia — a form of hair loss caused by physical pulling of the follicle (Mayo Clinic, 2026; AAD, 2023). Unlike most other forms of hair loss, traction alopecia is entirely preventable by loosening hairstyles before permanent follicular scarring occurs.
Is Hair Loss Preventable?
The honest answer depends on the cause. Most hereditary hair loss — driven by DHT and genetics — is not preventable (Mayo Clinic, 2026). However, treatment started early can significantly slow the process. FDA-approved options like minoxidil (Rogaine) and finasteride (Propecia) have demonstrated efficacy in slowing hair loss and in some cases stimulating regrowth (Healthline, 2024; Phillips et al., 2017). For a detailed look at how these treatments compare and what the evidence actually shows, see our hair loss medications guide.
For non-hereditary causes, prevention is often very much possible: eating a nutrient-dense diet, managing stress, treating underlying medical conditions, and choosing gentler hairstyles can all meaningfully reduce hair loss risk (AAD, 2023; Mayo Clinic, 2026).
When Should You See a Doctor?
See a healthcare provider — ideally a dermatologist — if you notice sudden or patchy hair loss, shedding accompanied by scalp pain or itching, or hair loss following a new medication or significant health event (Mayo Clinic, 2026). Early intervention generally yields the best results, regardless of cause.
The Bottom Line
The main cause of hair loss in men is androgenetic alopecia — a hereditary condition driven by genetic sensitivity to DHT that causes progressive follicular miniaturization over time. It affects tens of millions of men and is responsible for the vast majority of male pattern baldness cases worldwide. But hair loss is rarely a single-factor story. Stress, nutritional gaps, medical conditions, autoimmune responses, and even the way you wear your hair can all compound or trigger hair loss independently.
Understanding the root cause — quite literally — is the first and most important step toward doing something about it.


Video: Watch a hair restoration specialist explain the DHT-follicle connection and what it means for treatment options.
It’s Not Just Genes: The Other Major Causes
While AGA is the leading cause, it doesn’t tell the whole story. Hair loss in men can also result from a range of other factors — some temporary, some serious. Here’s what the research says:

Telogen Effluvium: When Stress Pulls the Trigger
Telogen effluvium (TE) is considered the second most common form of hair loss seen by dermatologists (Healthline, 2023). It occurs when a significant physical or emotional stressor — think surgery, illness, extreme psychological pressure, or even COVID-19 — shocks a large number of hair follicles into the resting (telogen) phase of the hair growth cycle simultaneously (Phillips et al., 2017; Mayo Clinic, 2026).
The result? Handfuls of hair falling out, typically two to three months after the triggering event. The good news is that telogen effluvium is usually temporary. Once the stressor is resolved, hair typically regrows within six to nine months (AAD, 2023; Healthline, 2023). The bad news: chronic stress can turn what was once a temporary issue into a long-term problem.
Nutritional Deficiencies: You Are What You Eat — Including Your Hair
Your hair follicles are among the most metabolically active structures in the body. They require a constant, adequate supply of nutrients to maintain healthy growth cycles. Deficiencies in iron, zinc, protein, biotin, vitamin B12, and vitamin D have all been linked to hair loss and disrupted hair growth (AAD, 2023; Healthline, 2024).
According to Guo and Katta (2017), nutrient deficiency plays a meaningful role in hair loss, with iron deficiency being particularly prevalent among those experiencing diffuse shedding. The key takeaway: a nutritional gap doesn’t cause male pattern baldness, but it can dramatically accelerate it or trigger a separate shedding event altogether. If you’re looking to address this proactively, understanding the essential nutrients your follicles actually need is a good place to start.
Thyroid Disorders and Medical Conditions
Your thyroid gland produces hormones that regulate metabolism — and when those hormone levels are off, your hair pays the price. Both hypothyroidism (underactive thyroid) and hyperthyroidism (overactive thyroid) can cause diffuse hair thinning and loss (Mayo Clinic, 2026; Healthline, 2024).
Other medical conditions associated with hair loss include lupus, scalp psoriasis, polycystic ovary syndrome (PCOS) in women, and sexually transmitted infections like untreated syphilis (AAD, 2023).
Alopecia Areata: When the Immune System Turns Against You
Alopecia areata is a distinct autoimmune condition in which the body’s immune system mistakenly attacks healthy hair follicles, resulting in sudden, patchy hair loss (Mayo Clinic, 2026; AAD, 2023). It can affect the scalp, eyebrows, eyelashes, and other body hair, and in severe cases can lead to complete hair loss on the scalp (alopecia totalis) or across the entire body (alopecia universalis). Unlike androgenetic alopecia, alopecia areata is not driven by DHT but by immune dysregulation.
Medications and Chemical Treatments
A number of commonly prescribed medications list hair loss as a side effect. These include anticoagulants, anticonvulsants, beta-blockers, oral retinoids, and certain antidepressants (Healthline, 2024; Phillips et al., 2017). Hair loss related to medication typically resolves once the drug is discontinued, but always consult your doctor before stopping any prescription medication. For a fuller breakdown of which drugs are most commonly implicated, see our guide on prescription drug hair loss in men.
On the styling side, harsh chemical treatments — relaxers, perms, bleaching agents — can damage the hair shaft and, over time, scar hair follicles, leading to permanent loss (AAD, 2023).
Traction Alopecia: Your Hairstyle Could Be the Problem
If you regularly wear your hair in tight braids, man buns, or cornrows, the sustained tension on the hair shaft can cause traction alopecia — a form of hair loss caused by physical pulling of the follicle (Mayo Clinic, 2026; AAD, 2023). Unlike most other forms of hair loss, traction alopecia is entirely preventable by loosening hairstyles before permanent follicular scarring occurs.
Is Hair Loss Preventable?
The honest answer depends on the cause. Most hereditary hair loss — driven by DHT and genetics — is not preventable (Mayo Clinic, 2026). However, treatment started early can significantly slow the process. FDA-approved options like minoxidil (Rogaine) and finasteride (Propecia) have demonstrated efficacy in slowing hair loss and in some cases stimulating regrowth (Healthline, 2024; Phillips et al., 2017). For a detailed look at how these treatments compare and what the evidence actually shows, see our hair loss medications guide.
For non-hereditary causes, prevention is often very much possible: eating a nutrient-dense diet, managing stress, treating underlying medical conditions, and choosing gentler hairstyles can all meaningfully reduce hair loss risk (AAD, 2023; Mayo Clinic, 2026).
When Should You See a Doctor?
See a healthcare provider — ideally a dermatologist — if you notice sudden or patchy hair loss, shedding accompanied by scalp pain or itching, or hair loss following a new medication or significant health event (Mayo Clinic, 2026). Early intervention generally yields the best results, regardless of cause.
The Bottom Line
The main cause of hair loss in men is androgenetic alopecia — a hereditary condition driven by genetic sensitivity to DHT that causes progressive follicular miniaturization over time. It affects tens of millions of men and is responsible for the vast majority of male pattern baldness cases worldwide. But hair loss is rarely a single-factor story. Stress, nutritional gaps, medical conditions, autoimmune responses, and even the way you wear your hair can all compound or trigger hair loss independently.
Understanding the root cause — quite literally — is the first and most important step toward doing something about it.


